What Is Gastric Cancer & What Are The Early Signs?
The incidence of gastric cancer – a disease in which malignant cells form in the lining of the stomach – is on the increase – in some cases unhealthy diets, an overabundance of processed foods and excessive levels of alcohol can contribute to the development of cancer, however, in many cases no obvious causes are ever determined.
Unfortunately, one of the main problems with gastric cancer is the fact that, in the early stages, the symptoms resemble other, less serious or sinister conditions.
Symptoms
There may, for example be indigestion and stomach discomfort or a bloated feeling after eating. This may be accompanied by mild nausea, heartburn and a loss of appetite. Naturally, these symptoms are all ‘innocent’ in themselves.
In the more advanced stages of gastric cancer, the following symptoms may become apparent:
- Feeling full quickly
- Weight loss without trying
- Blood in stools (poo)
- Vomiting
- Stomach pain
- Difficulty swallowing
Diagnosis
In order for a diagnosis of gastric cancer to be made, the following tests and procedures may be used:
- Physical exam and health history: your GP will carry out an examination of your body to check your general signs of health, and will check for signs of disease, such as lumps
- Blood tests: you may then be referred testing
- A general blood count will then be carried out. This involves a sample of blood being drawn and checked for the number of red and white blood cells and platelets
- An upper endoscopy may be carried out to look inside the oesophagus, stomach and duodenum (the first part of the small intestine) to check for abnormal areas. At this point, an endoscope (a thin, lighted tube) is passed through the mouth and down the throat into the oesophagus.
Post diagnosis
If a cancer diagnosis is made, then other tests will be done to find out if the cancer cells have spread within the stomach or to other parts of the body.
If the cancer has spread, this is known as metastasis. This means that cancer cells have broken away from where they began, ie, the primary tumour, and travel through the lymph system, or through the blood.
Treatment
Surgery is a common treatment of all stages of gastric cancer. This can range from subtotal gastrectomy, which involves removal of the part of the stomach that contains the cancer and nearby lymph nodes, to total removal of the entire stomach, nearby lymph nodes and parts of the oesophagus, small intestine and other tissues near the tumour.
Other treatments may include:
- Chemotherapy: this is a treatment that uses drugs to stop the growth of cancer cells, either by killing the cells, or by stopping them from dividing. A type of chemotherapy currently being studied to treat gastric cancer is intraperitoneal chemotherapy, in which the anticancer drugs are carried directly into the peritoneal cavity (the space that contains the abdominal organs) through a thin tube.
- Radiation therapy: this therapy uses high-energy X-rays or other types of radiation to kill cancer cells or keep them from growing.
Unfortunately, while gastric cancer is on the increase, there’s also an increasing link between gastric cancer and oesophageal cancer. That’s because it can sometimes be difficult to tell the difference between stomach, oesophageal and the associated gastro-oesophageal junction (GOJ) cancer.
Gastro oesophageal junction (GOJ) cancer develops at the point where the oesophagus joins the stomach. Research suggests that GOJ cancer is a separate type of cancer that can behave differently to cancers of the oesophagus and stomach. Cancer is described as GOJ cancer if the centre of the cancer is less than 5cm above or below the gastro-oesophagus.
Oesophageal cancer is a cancer that’s found anywhere in the oesophagus – that’s your food pipe or gullet. Basically, it’s the long tube that carries food from your throat to your stomach.
As with gastric cancer, the number of people who develop this type of cancer is increasing.
In Northern Ireland in 2016, a total of 226 people were diagnosed with oesophageal (gullet) cancer. In the same year, 214 people were newly diagnosed with gastric (stomach) cancer.
Symptoms which indicate there may be cancer in the oesophagus are often vague and fairly common symptoms and therefore can be overlooked. However, as with any other area of your body, any changes, however subtle, if persistent should not be ignored.
No one knows what causes all GOJ cancers, but there are some factors that may increase your risk of developing it.
Being very overweight (obese), for example, and having chronic gastro-oesophageal reflux are both risk factors for GOJ cancer.
Barrett’s oesophagus can also increase your risk of type 1 GOJ cancer. Barrett’s oesophagus is a condition where the cells lining your oesophagus have become abnormal, and usually happens due to long-term acid indigestion (acid reflux).
The most common treatments for gastro oesophageal junction cancer are:
- Surgery
- Radiotherapy
- Chemotherapy
- Chemotherapy and radiotherapy together (chemoradiotherapy) Targeted cancer drug treatment
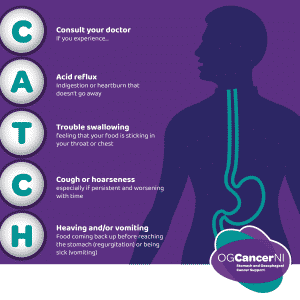
When to seek help
If you have any of the following symptoms, you should see your local doctor and discuss them further:
- Swallowing difficulties or a sensation of food sticking in your chest
- Pain or discomfort as food passes down the oesophagus
- Persistent heartburn/acid reflux (persistent would be 2 to 3 weeks without passing off)
- Persistent cough or hoarseness
- Persistent hiccups
- Regurgitation of food on a regular basis
- Persistent nausea/retching/heaving
- Unexpected weight loss/unusual tiredness
Your GP may initially give you a medication to see if that can solve your symptoms, but if, after two to three weeks, your symptoms have not gone away, he/she may refer you for an endoscopy.
This is a camera which is passed down your oesophagus (with sedation if you prefer) where the endoscopist can have a look at the lining of the oesophagus and the stomach. They may take biopsies if they are unhappy about anything they see. This does not necessarily mean you have cancer; it may be that they have seen some ulceration or other changes in the normal linings.